 A radionuclide bone scan or MRI can be used to screen for stress fractures. Later, once the fracture has been around long enough, periosteal reaction is often seen adjacent to the fracture site. If the fracture is fairly new, then there may be no plain film evidence of it. However, this is more likely in certain bones, such as the tibial shaft, the metatarsal shafts, the femur, and the bones of the pelvis. With chronic repetitive stress, one can break any bone in the body. A computer attached to the device then takes this data, and uses it to create a transmission image of the bones of interest, and then compares this data with normative standards so that one can decide if the patient indeed has osteoporosis. If less bone is present, then more X-rays make it through. If a patient has more bone, then less X-rays make it through the patient into the X-ray detector. As this scanning arm moves about, a beam of X-rays at primarily two different energies are transmitted through the patient, and their respective amounts of absorption by the tissues of the patient’s body are measured by a sensing probe on the other side of the patient. A scanning arm then passes over the patient and scans the area of interest. This is done with a dedicated device about the size of a conventional radiographic examination table. The current state of the art in quantitative bone assessment is dual energy X-ray absorptiometry (DEXA). To definitively diagnose osteoporosis, one must perform some type of quantitative imaging study on the bone in question. If less that 30 – 50 % of the bone is gone, then you may have trouble being sure that osteoporosis exists at all. If the osteoporosis is really bad, the bones may look washed out, and only the primary weight-bearing trabeculae may be visible. In order to see a lesion in bone, an estimated 30 to 50 % of the bone must first be lost. Now, how do you go about diagnosing osteoporosis? Well, if it is early osteoporosis, looking at radiographs won’t help you much, because plain films are hideously insensitive to osteopenia. Other risk factors for osteoporosis include Caucasian heritage, smoking, lack of antigravity exercise, low dietary calcium intake, and various amenorrheic states. This is especially true of postmenopausal women, who may lose up to 20 % of their bone mass in a year in extreme cases. Osteoporosis lies in wait for every living human, if only they live long enough to develop it. This is by far the most common reason for a fracture without significant trauma. 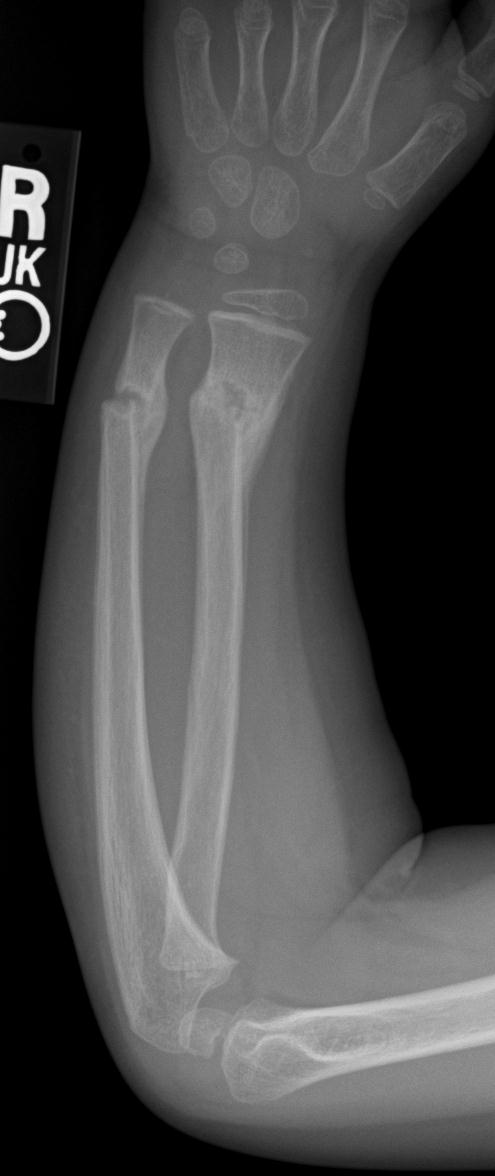
When there is normal bone but just not enough of it, we call it osteoporosis. Therefore, one should also consider infection, osteomalacia, and Paget’s disease, among other causes. However, almost any underlying process of bone that weakens the bone can lead to a pathological fracture. Probably the most common cause of this is an underlying tumor, either benign or malignant. 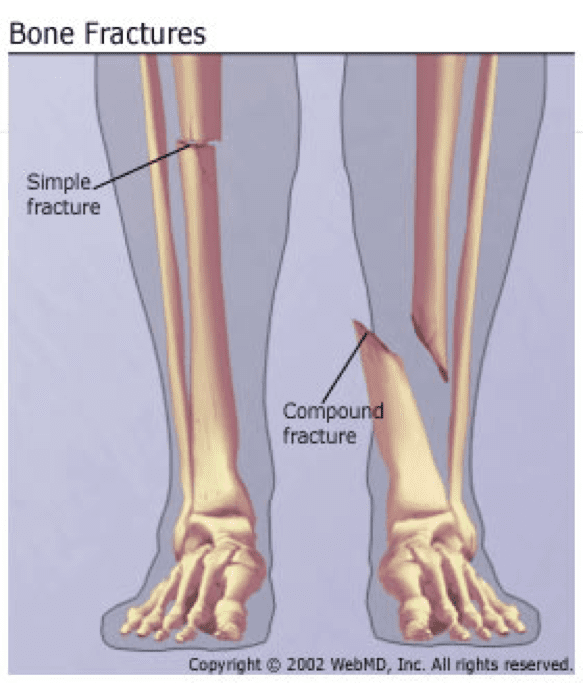
To do this, you must first answer two questions: 1) did the fracture occur through normal or abnormal bone 2) is there normal or decreased amount of bone present? Once you have answered these two questions, you can use the following handy-dandy flowchart to arrive at the most likely mechanism for the fracture.įractures through abnormal bone are called “pathological” fractures. If there is no evidence of such a force, we must look for some other reason. Usually, that reason is that a substantial force has been applied to the bone. The thing to remember is that a bone needs a reason to break. Generally, the differential diagnosis here is fairly logical. Whenever you get this history, a red flag should pop up in your visual cortex and a bell should go off in your auditory tracts. The circumstance of fracture without any history of significant trauma is not uncommon. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
